Researchers at the Icahn School of Medicine at Mount Sinai have gained a deeper understanding of the nuanced roles of JAK inhibitors, or modulators, in inflammation across various cell types and tissues. Their findings suggest a more precise approach is required to potentially expand JAK inhibitor use to a wider range of allergy and inflammatory disorders. Details on the findings were published in the December 21, 2023, issue of the journal Cell.
JAK1 is a key protein in the body that supports cell communication and controls the immune system.
It is part of a group of proteins that pass signals from a cell’s exterior to its interior.
Controlling JAK1 activity is also important in managing conditions such as rheumatoid arthritis and some cancers.
Current JAK inhibitors work well against inflammation in diseases like eczema, but the study suggests a need for a nuanced approach in modulating JAK activity for conditions like asthma.
The potential shift toward enhancing, rather than blocking, JAK activity in lung neurons could be a transformative strategy, distinct from traditional JAK inhibitors that mainly target immune cells, say the investigators.
As part of the work, a mouse made with a patient-specific mutation in the gene for JAK1 revealed how this mutant protein causes disease and how it could potentially be harnessed for broader therapeutic use.
The study showed that activated JAK1 signaling has tissue-specific effects, including an unexpected immunoregulatory role in lung sensory neurons, where it suppresses lung inflammation.
“This may explain why JAK1-selective inhibitors, while highly successful in atopic dermatitis, have not advanced for asthma treatment and implies that JAK1 signaling has varying or even opposing effects in different cell types and tissues,” says lead study author Brian Kim, MD, MTR, FAAD, the Sol and Clara Kest Professor of Dermatology, Vice Chair for Research, and Director of the Mark Lebwohl Center for Neuroinflammation and Sensation at Icahn Mount Sinai.
The study involved a type of JAK1 gain-of-function (GOF) mutation, first reported by study co-author Stuart Turvey, MBBS, DPHIL, FRCPC in 2017, from patients with an immune dysregulatory and hypereosinophilic syndrome characterized by severe eczema and asthma.
A JAK1 GOF mutation is a change in the gene that encodes the JAK1 protein, making it more active than normal.
This increased activity can lead to overactive immune responses and may cause health problems like autoimmune diseases or cancer.
“As a pediatrician, I started this work with a commitment to finding a diagnosis and treatment for a family where three members had severe eczema, asthma, and other allergic manifestations. It turned out that they were the first people in the world recognized to have a genetic change causing gain of function of JAK1,” says Dr. Turvey, Professor, Division of Immunology, Department of Pediatrics, Faculty of Medicine, and Canada Research Chair in Pediatric Precision Health, BC Children’s Hospital and The University of British Columbia, Vancouver, Canada.
“Today’s publication, led by Dr. Kim and his team at Mount Sinai, is a powerful example of globally collaborative translational research where they started with this single family and have now generated fundamental insights into the interactions between the human immune system and the nervous system. This is precision medicine in practice.”
Previous research by Dr. Kim and his team revealed that JAK1 signaling, typically responsible for regulating immune cells’ inflammatory response, is also present in neurons and controls the sensation of itch.
In their new study, Drs. Kim and Turvey created mice with the same genetic mutation as the patients to better understand why JAK1 inhibitors work for some allergy and inflammatory conditions.
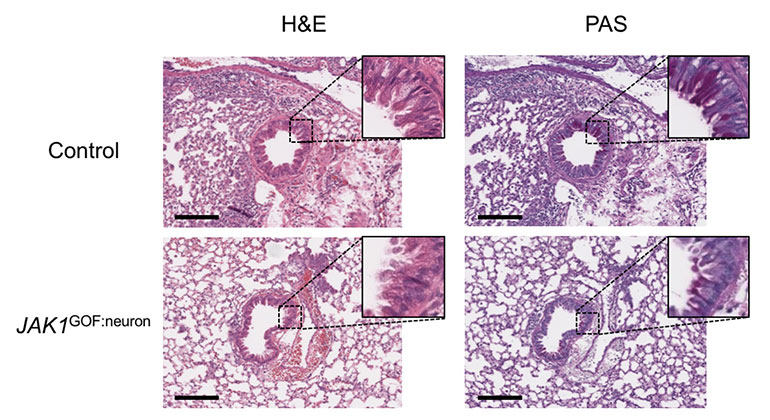
In the lung neurons of the mice, the JAK1 mutant protein reduced inflammation caused by exposure to mold by producing substances that suppress inflammation.
However, the mice still showed the same skin condition as the original patients, indicating that JAK1 signaling has different effects in different cells and even within the same cell type in different parts of the body.
“Better understanding of JAK signaling in different parts of the body not only helps us discover new things about biology but also gives us a glimpse into how JAK medicines might be used in the evolving landscape of innovative treatments,” says Dr. Kim.
Next, the researchers plan to examine how additional genes along the JAK pathway may also inform tissue-specific patterns of disease. “For example, another protein called STAT6 is further downstream of the JAK1 pathway. Dr. Turvey has found patients with mutations in these genes who also develop similar allergic conditions. However, whether these specific mutations can inform therapeutic strategies for specific diseases remains a very exciting field of inquiry,” says Dr. Kim. https://www.mountsinai.org/about/newsroom/2023/new-insights-revealed-on-tissue-dependent-roles-of-jak-signaling-in-inflammation






Recent Comments